Macrophage extracellular traps promote maladaptive cardiac remodelling and heart failure via PAD4-dependent mechanisms
Macrophage extracellular traps promote maladaptive cardiac remodelling and heart failure via PAD4-dependent mechanisms
Ichimura, S.; Misaka, T.; Okochi, S.; Ogawara, R.; Sato, Y.; Miura, S.; Yokokawa, T.; Miura, S.; Ueda, K.; Oikawa, M.; Yoshihisa, A.; Ikeda, K.; Ishida, T.; Takeishi, Y.
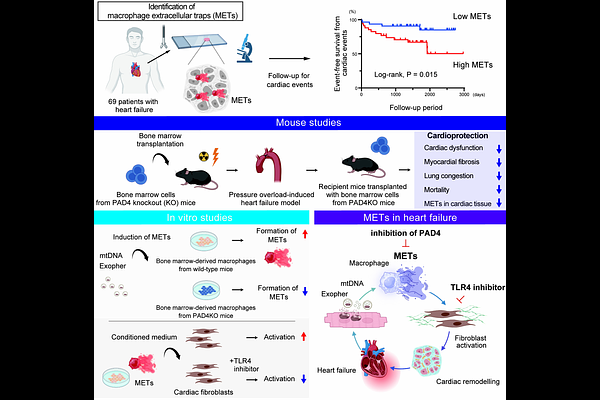
AbstractAims The activation of inflammatory cells, particularly macrophages, plays a pivotal role in the pathogenesis of cardiac remodelling and heart failure. Emerging evidence indicates that extracellular traps released from inflammatory immune cells contribute to the progression of various pathologies. However, the clinical relevance and mechanistic role of macrophage extracellular traps (METs) in heart failure remain to be elucidated. Methods and Results Endomyocardial biopsy specimens from 69 patients with heart failure were analysed by fluorescent immunostaining to identify and quantify METs. The numbers of METs per myocardial tissue area in patients with heart failure showed a negative correlation with left ventricular (LV) ejection fraction and a positive correlation with LV end-diastolic diameter. Patients with higher MET counts had significantly lower event-free survival from the composite cardiac events. In a murine model of pressure overload by transverse aortic constriction (TAC), METs were most abundantly observed at 3 days post-TAC and remained detectable throughout the 4-week observation period. In vitro, time-dependent MET formation was induced by an intrinsic trigger of mitochondrial DNA in bone marrow-derived macrophages from wild-type (WT) mice, but not in peptidyl arginine deiminase 4 (PAD4)-deficient macrophages, indicating that PAD4 activity is indispensable for MET formation. The recipient mice transplanted with bone marrow cells from PAD4 knockout mice showed more preserved cardiac function, reduced myocardial fibrosis, and improved survival in response to TAC, compared to those transplanted with WT mice. Ex vivo analyses demonstrated that conditioned medium containing METs from WT macrophages induced fibroblast-to-myofibroblast transition via Toll-like receptor 4 signalling. Conclusions PAD4-dependent MET formation from bone marrow-derived macrophages represents a novel driver of cardiac remodelling. Targeting MET formation may offer a potential therapeutic strategy for heart failure.