A treatment-resilient lipid metabolic program drives temozolomide resistance in glioblastoma
A treatment-resilient lipid metabolic program drives temozolomide resistance in glioblastoma
Naghibzadeh, K.; Barzegar Behrooz, A.; Kavoosi, M.; Cordani, M.; Los, M. J.; Pecic, S.; Vitorino, R.; Vitorino, C.; Ravandi, A.; Shojaei, S.; Ghavami, S.
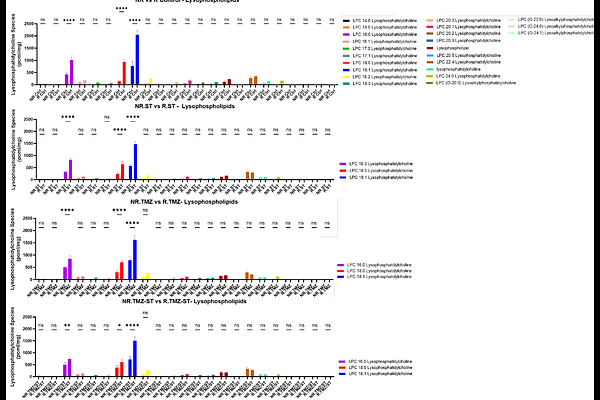
AbstractTemozolomide (TMZ) resistance remains a major obstacle in glioblastoma (GBM) therapy, yet the metabolic adaptations underlying this phenotype are incompletely understood. Here, we performed integrative lipidomic, ultrastructural, and pathway analyses to define lipid metabolic reprogramming associated with TMZ resistance and failure of statin-mediated sensitization. Targeted LC-MS lipidomics quantified 322 lipid species across 25 lipid classes in TMZ-sensitive and TMZ-resistant U251 cells under basal conditions and following TMZ, simvastatin, or combination treatment. Multivariate analyses (PCA, PLS-DA, and volcano plots) revealed a robust and treatment-resilient lipidomic signature in resistant cells characterized by enrichment of lysophospholipids, sphingolipids, and cholesteryl esters, alongside depletion of glycerolipid and phospholipid pools. Complementary univariate analysis confirmed these changes at the species level, demonstrating consistent elevation of lysophosphatidylcholine/ethanolamine, glycosphingolipid subclasses, and cholesteryl esters, together with reductions in phosphatidylcholine, phosphatidylethanolamine, phosphatidylinositol, and diacylglycerol intermediates across multiple treatment conditions. In contrast, sensitive cells displayed dynamic lipid remodeling, including phosphatidylinositol and phosphatidylethanolamine enrichment associated with autophagic membrane expansion. KEGG pathway analysis linked the resistant phenotype to Rap1, PI3K-Akt, and phospholipase D signaling networks regulating vesicle trafficking and membrane homeostasis. Transmission electron microscopy confirmed a vesicle-rich intracellular architecture consistent with persistent autophagy flux blockade in resistant cells. Collectively, these findings define a stable lipid metabolic program characterized by lysophospholipid expansion and cholesteryl ester accumulation that supports membrane integrity and therapeutic resistance. Targeting lipid buffering and cholesterol storage pathways may represent a promising strategy to overcome chemoresistance in glioblastoma.